The birth story of my Second Baby.You can read about the birth of my first baby, Morgan, in the original Nostalgia blog here. I wrote this one a bit differently, as a letter to my younger daughter about her birth. Some of the details are forgotten, out of order, but they are how I remember experiencing it. I honor this version of these memories. Aria Leigh 5 days past our due date. November 6th. How we’ve been waiting for you. I didn’t have to experience this limbo phase with your sister, she came promptly on her due date. The beautiful encouraging things I say to my doula clients seemed so silly to say to myself. I posted in the Doula Facebook group for my peers to say those sweet words to me, and one of my friend’s responses was the following poem; I now send it to my all my clients on their due date. “Waiting Dear Baby, here beneath my heart, I thought you might come today; The timing seemed just right. But the stars are out And the moon is high And sheepishly I wonder why I try to arrange the plans Of God. For now I know You will not come Until the one who holds eternity Rustles your soft cocoon And whispers in tones that I will not hear, ‘It’s time, precious gift.’ ‘Now it’s time.’
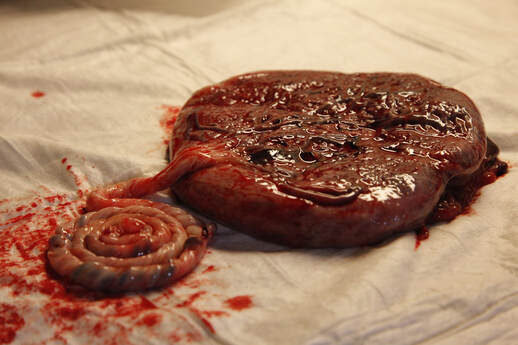
The day started out like any other, you were still moving around like your comfy, happy self, NEVER to be leaving my body. Morgan and I went to Towson to vote. The voting people were very nice about allowing me to sit in a chair whilst a stand-in kept my spot in line. They all casually asked me “oh when are you due?”, with the surprised shocked face when my response was an equally casual, a few days ago. We got home around 1pm with our new ‘I Voted’ accessory stickers. I messaged Daddy that I was spotting a bit, I was nervous, and the kitchen wasn’t clean. He asked me if he should come home and clean. Having been having contractions and loss of mucus plug for weeks, I responded that this was going to be just nothing just like every other time. Not a half hour later I resigned to this might actually being it. We hadn’t worked on causing the contractions at all, these felt different, and with every contraction I lost more mucus plug. There was quite the back and forth about whether Daddy should stay at work, or go vote. He figured he wouldn’t be in the next day, or for the following few weeks so he needed to get his work done. With contractions coming about every 7-8 minutes apart, and having to stop and breath through them. I told daddy I thought it was funny that I was sad this would be the last day I was pregnant. All this wanting you to arrive and give birth, and now I was sad for this transition. Still continuing to debate Jake’s schedule. Trying to really feel and be happy and believe that I’m in labor. At 5:15 I messaged Daddy to say yes “We’re for sure in labor”. His response was that he was excited and loved me, and was coming home. He got home around 6pm, to find me having contractions still about every 6-7 minutes apart. I don’t really remember if I made dinner, I assume we ate something. The surges were intense but easily manageable, especially with my TENs unit. Goodness to not have back labor from a posterior baby, I could give birth like that a million times over. You’d been continually hanging out ROA, not as ideal as LOA, but I’ll take it. I felt called to do an inversion, to help make sure you had space to tuck your head and rotate freely through the cardinal movements. Morgan and Carter, our corgi, joined me in my task. I wonder if Carter knew what was going on again, he had been such a beautiful support at your sister’s birth. Thinking I still had a long way to go, we wanted to keep going with our usual evening routine, so Morgan and I took a bath together. I love your sister so much, and I had wanted her to be at your birth, but her not even four year old self could not grasp the concept of being SILENT during contractions. She’d still whisper, and try and talk to me about inane things. I couldn’t handle both the contractions and the talking. I love this picture, and the way she was looking at me during a contraction, so young and small, but still so knowing and questioning. ,Daddy got Morgan to sleep while I continued to labor in the bathtub. It was around 9pm when he was finally back, Mo content to sleep in her bed. My doula brain was apparently completely turned off at this point. Looking back, it is so clearly obvious I was in transition; reaching the complete surrender phase that I’ve seen so many birthing people meet before. The fear, the overwhelm, the standing on the edge about to fall feeling. I was having almost back to back contractions at this point and shaking uncontrollably. Crying that this was going to be just like Morgan’s birth. I was going to be stuck, not making it past 4cms, having my body do all this work to have made basically zero progress, and still have all night to go. Jake called our Midwife, Deanna, to update her. I think she asked him if I wanted her to come, to which again my crying response was that it’d be pointless, I was nowhere near ready. Being the wonderful midwife she is, I have a feeling she didn’t listen to me, as the next time we called not a half hour later, she was almost at our house. Jake thought it was time for me to get out of the tub, with all the shaking and crying. It seemed I couldn’t get grounded it the water, and I needed to reset out of it. I got dried off and moved to the sofa in the sunroom. I put my TENs back on, and things started to feel a bit calmer. Time gets very fuzzy after this, but it must have only been about 15 minutes. I thought my water might have broken, but it was only a small trickle. We called Deanna to tell her. The worse labor felt was through these next 10-15 minutes. Daddy had left again to try and get the birth pool filled. We had called the midwife again to tell her that I had started to feel pushy, but she was only a few minutes away. Remember the smart midwife that ignored my clear denial? Tova, the birth assistant and Deanna arrived; I don’t remember who first. Tova tried to listen to the baby’s heartbeat with the doppler, but even just the slightest pressure on my stomach and my pain increased, and tolerance of labor decreased greatly. This is a part of home birth I like immensely – there are no “have to’s”, I don’t know if they actually ever got a heartbeat during labor, but I felt fully supported, safe, and my body’s ability honored. They realized we didn’t have an attachment for the hose. I thought we had checked this prenatally, but these things happen. When we realized it was also probably pointless because it wouldn’t be remotely filled in time anyways, Jake finally came back over and laid with me on the sofa. I want my next birth to be full of this moment. All the sudden the overwhelming intensity went away. A wave of calm, grounded love washed over me and I know this is the energy you were born with. I was quiet through the next couple contractions, and could feel my body pushing you out. It still baffles me that some providers seem to not believe an ejection reflex exists, it is so primal and there is no stopping it. Because I attend primarily hospital births, I’ve seen too much. Coached pushing, Pitocin contractions, all of these things that cause birth to be more dangerous. Even as much as I know the body wouldn’t be pushing unless it was ready, I couldn’t get the fact that we “hadn’t checked” out of my head. I said this to Tova, and she very wisely reminded me that my body wouldn’t be pushing unless it was ok, that even if there was a bit of cervix left, the pushing might help to push it completely out of the way. It was just the reminder and reassurance I needed to fully embrace and dive into the final stage of labor. I felt the surge of adrenaline that accompanies this transition. I needed to stop laying down and get up and active. I sat on the edge of the sofa, Jake between my legs. I felt you drop down fully through my pelvis – both internally and externally. All the sudden the lower part of my stomach was squishier than it had been in a very long time. A huge surge took over, and my water burst all over your daddy… oops. I know he went and changed, but I didn’t really recognize he had left. I honestly don’t know why, if it was a suggestion, or I felt the need to change position. But we put some trash bags over some pillows and I kneeled on the floor leaning over the sofa. Your daddy behind me, ready to catch you. I felt your beautiful body wiggling down. Your head applying pressure at my opening. I became very fearful of tearing, I hadn’t torn with Morgan but I did have skid tears at the top of my labia. I reached my hand down to feel your head and support myself. This gave me the extra confidence I needed to feel that my body was indeed stretching and not tearing. I know had I been in a hospital, or even some birth center or home births, I would not have felt comfortable reaching down knowing a bunch of people were looking at me with bright lights or flashlights. I felt dark and protected, I felt intimate with Jake, like we were in our own little bubble birthing you into this world. For my next birth I would love for someone to remind me to GO SLOW. Because once your tiny head was exiting there was an overwhelming feeling that the rest of you had to come out immediately too. Your shoulders got held up a bit, as you really did need time to turn more, but Daddy was right on top of it, listening to me saying your shoulders weren’t out yet. I know he used his fingers to stretch me a bit more and turn you to come out. Having had other cervical exams with Morgan’s pregnancy and birth, I can say that it being Jake’s fingers and not a stranger made me not tense up horribly about it. I felt love, support, and sexuality. I felt every inch of your body sliding out of me. It was completely orgasmic. I am 100% for immediate skin to skin, had that with your sister, and honestly hated it. I was so done with sensation, so done being touched, so done with this baby who had caused me such horrific pain. I wanted nothing to do with her being on my chest, I just wanted a minute to breathe. We took a birth pause with you. Your daddy held you while I took a minute. I remember looking at Tova who was next to me, and her just smiling this knowing smile. The one I know I give my clients, the one that just says, “Yes. Yes, I’ve been here too. I’ve witnessed this too. Welcome, sweet new soul.” 10:39 pm When I was ready, I turned over and held you on my chest. I remember saying “Hi, you really do exist.” You were covered by a blanket, and it took me a little bit to be curious about whether you were a boy or a girl. A healthy, stunning, baby girl. Your head had no molding to it, evidence to the very limited time I pushed. Carter came over to check out our new addition to the family. His energy between Morgan’s birth and yours is so funny to me. An older, wiser, experienced baby supervisor. He came and smelled you, licked you, and went back to bed. As if to say I’ve known you’ve been coming, I’m happy you’re here, and I’ll watch you more in the light. I birthed the placenta. I honestly can’t remember who or when the cord was cut. No tears. You latched and settled immediately. Tova weighed and measured you. I love the way she handled you, with such respect and delicate care. Again, different than the hospital, where the nurses are so used to handling baby’s they forget you’ve never even been touched before. That you are unique and individual, and your great newness needs to be honored. We got cleaned up and tucked into bed. Tova read us postpartum instructions, but they’d be by again soon. There are so many fantastic things about a home birth, but one of the best is that you are immediately home. Your bed, your sounds and smells, your pillows, your love and space. We nursed again, and I laid down with you right next to me safely set up to bed share and fell asleep, probably only around 1 or 2 am. Your daddy was very spoiled in that he only had to be a labor support for about 4 hours, we’ll see if he’s as spoiled the next time, that’s less time than any of my doula births I’ve been to! In the morning you got to meet your sister! She was and still is very excited about you. We also messaged the family that you had arrived last night. It was a wonderful intimate peace to keep that you had been born to ourselves for a bit, as much as everyone hated it. The rest of the family came by to meet you throughout the day I encapsulated your placenta, with a beautiful marginal cord insertion of a very spiraled cord. It was so cool, I’ve not seen many cords with such a pattern. It’s December 4th, 2019, well over a year since your birth. The details have faded, but I felt the need to get it all down before the birth of your younger sibling occuring in a few weeks. We never expected to get pregnant so soon postpartum, but given how much you love your older sister, I think you’ll enjoy having another little one around. I loved giving birth to you. It healed so much of what my body had experienced with Morgan. I wish every birthing person could experience the purest ease of labor and birth that was your arrival. It was orgasmic, intimate, supported, and so full of pleasure and love. I wouldn’t have called any of it painful, just incredibly intense. I’m looking forward to the next birth. Thank you for giving me the confidence and excitement, and for coming into our lives when we needed you. I love you dearly. Thank you to our wonderful birth team!!
Our midwife - Deanna Kopf of Birthwise Midwifery Birth Assistant and soon to be Midwife of her own! - Tova Brody of Tova Brody Birth Chiropractor - Dr. Pam of First Step Chiropractic
0 Comments
Postpartum DepressionPostpartum depression is not showering until the afternoon. Postpartum depression is cleaning the kitchen before your partner gets home so it looks like you have your shit together. Postpartum depression is debilitating. Postpartum depression is getting furious that the tiny dictators need something from you, yet again. Postpartum depression is screaming into a pillow for it all to just stop. Postpartum depression is the guilt others make you feel for not loving every second of your precious miracle's mundanity. Postpartum depression is feeling like you're a constant failure. Postpartum depression is feeling like a horrible mother. Postpartum depression is wishing you weren't even a mom. Postpartum depression is drowning in sorrow at the negativity. Postpartum depression is isolating. Postpartum depression makes it nearly impossible to get out of the house - see again isolating. Postpartum depression causes such worry that you're ruining your children's happiness. Postpartum depression is hating society for being set up in a way that makes you raise your children essentially alone. Postpartum depression is missing the help of your partner so much your heart physically hurts. Postpartum depression is hating that the only thing that seems to make your child happy is their father being home. Postpartum depression is incredibly unfair. Postpartum depression. How we hate you. Postpartum depression effects as many as 1 in 5 people up to 1 in 9 people. Postpartum depression is treatable. Postpartum depression does not define who you are as a person or parent. Your beautiful body grew and birthed your baby, either through a vaginal birth or belly birth. Showing connection and love to your now solo body can be challenging, especially if your birth experience was not what you had envisioned or traumatic. If you are suffering from any lingering panic, depression, anger, dissociation, or inability to bond with your family or self, please reach out to a therapist. Contact any doula in your area and they will have a recommendation of one that specializes in birth trauma and postpartum issues. When trying to reconnect to your body, it can be even more difficult if you are experiencing continued pain. PAIN IS NOT NORMAL. Pain is your body's way of telling you something is not right. Pain, numbness, dryness, random bleeding, tearing, or anything else that is anything other than happy healthy, is not normal. Inability to hold your bladder, sneeze, cough, laugh without peeing; is not normal! Again, a trip to a Pelvic Floor Physical Therapist will help fix this all up. If you're in the Baltimore, MD area Dr. Samantha Duflo of Indigo Physiotherapy is my favorite. At the end of your pregnancy journey, a baby, an organ, and a lot of blood came out of your vagina or your belly. Then you're an extra hot mess with your granny panties, milk leaking, squishy self. Reconnecting to your womb as something sexual can seem like an impossible task. We hear so much about self care, but what about self love and self-sex? Wonder if your partner is feeling a loose vagina; go find out for yourself and see they're not. Wonder if the stitches left you altered; grab a mirror and look. Do all of this when you're ready and feel called to reopen this aspect of your body and life. Exploring your body and your postpartum intimate bits can go a long way towards claiming yourself back from birth and baby. The fabulous Layla Martin released a new guided meditation that is free and takes a whole 5 minutes. It can really help in reconnecting you to your pelvic organs. She calls it her Honey Pot Practice. The amount of warmth and love you can feel flowing through your hands is pure bliss. The triangle position of your hands allows the same benefits of skin-to-skin you had with your newborn. Our bellies can be such a source of negativity and shame in our current body image culture, the simple act of loving skin-to-skin contact can go a long way in feeling better and embracing your soul's new housing. This practice can help relieve pain, increase circulation and therefor healthy moisture, arousal, and pleasure during intimacy. Your body belongs to you. Love it, embrace it, and visualize it covered in honey.
To conclude the main points:
First and foremost, what is herpes and what are the risks of becoming infected? Genital herpes comes from the sexually transmitted herpes simplex virus largely as either HSV-1 or HSV-2. HSV-1 is typically seen as an oral infection, but can be transferred and cause a genital infection. HSV-2 is typically seen in the genitalia. HSV, when active can cause one or more sores that blister and break taking sometimes over a week to heal. Most people remain asymptomatic or mistake symptoms for another skin condition like acne. Even when no active lesions are present, the person still sheds the virus 10% of the time in consistently asymptomatic people, and 20% of the time in symptomatic people. According to the CDC 11.9% of people are known to be infected with the virus, but 87.4% of people who have the virus never receive a clinical diagnosis(CDC Herpes Facts, 2019). This is largely because the CDC no longer recommends proactively screening for herpes in a standard STD screen. They found that someone diagnosed when not having active symptoms will on average not change their sexual behavior such as wearing a condom or remaining abstinent (CDC Screening, 2019). |
Categories
All
Archives
December 2019
|

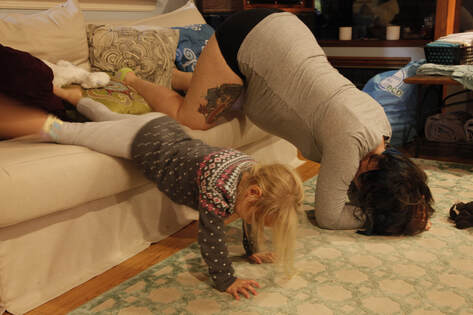









 RSS Feed
RSS Feed